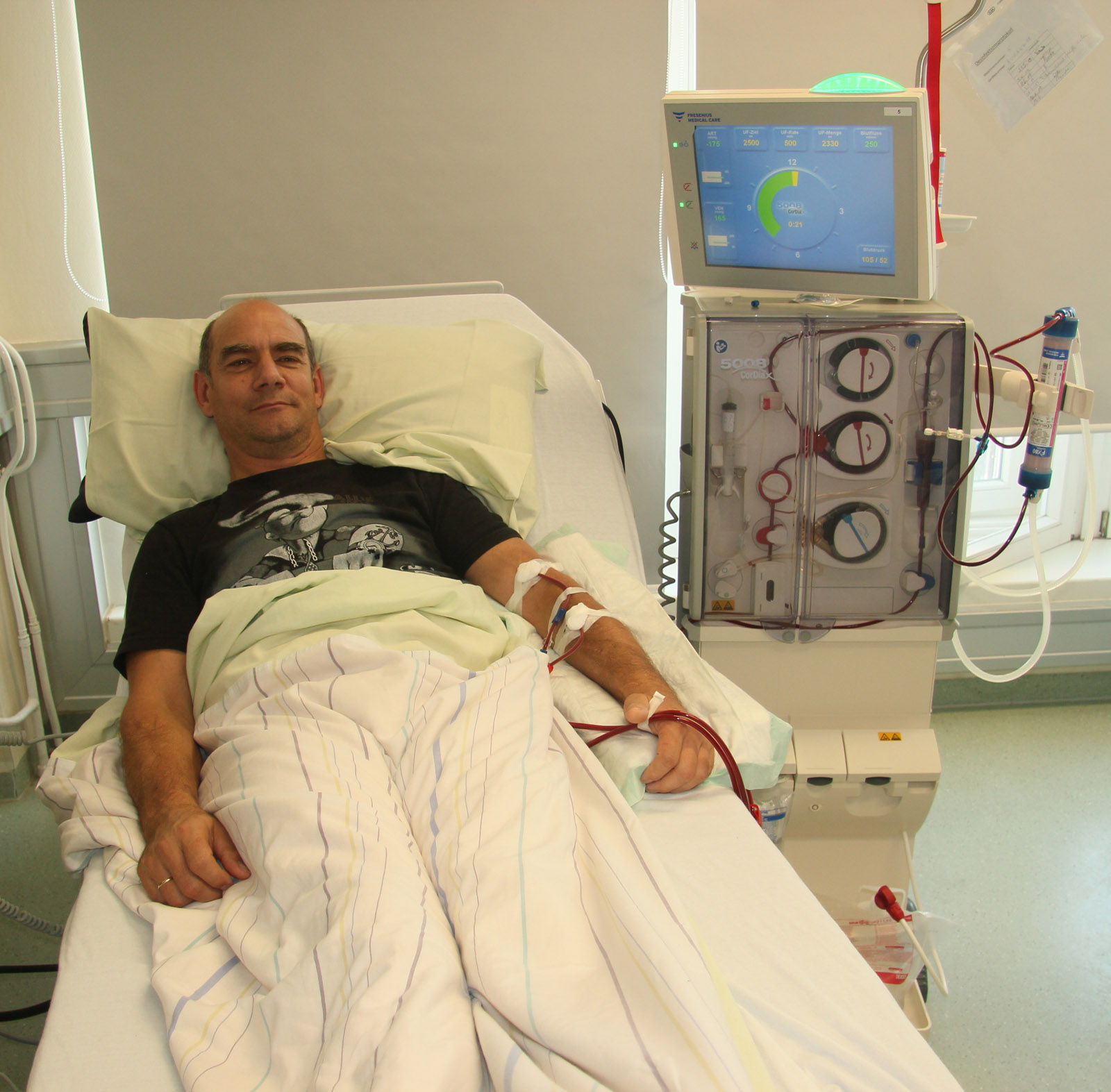
Some 90,000 people in Germany every year have to undergo dialysis three times a week for four to five hours, because their kidneys no longer function properly and cannot eliminate toxins sufficiently. During treatment harmful metabolites are removed from the blood by transferring them outside the body via a semipermeable membrane into a dedicated dialysis fluid called the dialysate. The pores of the membrane are so narrow that only toxins up to a certain size can pass them. Small molecules such as water, electrolytes and uremic toxins – urea, uric acid and creatinine – transit the membrane into the cleaning fluid, while large molecules such as proteins and blood cells are rejected. The entire blood is recirculated and cleared approximately three times per hour.
Dialysate can only be used once
For a dialysis treatment, approx. 400 liters of dialysate are required. Hospitals and dialysis centers prepare this water using reverse osmosis systems, which consume a lot of energy and are expensive. It is challenging that dialysate can only be utilized once, as it disappears as waste water after the blood purification treatment. To treat 90,000 patients per year this requires more than 5.6 million cubic meters of ultrapure water. In many regions of the world this requirement is not met. According to estimates, over a million people die every year by lacking access to dialysis.
“Dialysis water is precious. Germany’s one year dialysis water fills a 175m cube. Up to now there has been no cost-effective method to reclaim dialysate,” says Dr. Rainer Goldau, scientist at the Department of Extracorporeal Immunomodulation at the Fraunhofer Institute for Cell Therapy and Immunology IZI in Rostock, whose research work is focused upon this subject. The body approximately produces 25 grams of urea every day. This molecule – being of nearly the waters molecular size – also passes the filter membrane into the dialysate. The reverse osmosis technique, employed to generate potable water, does not have a sufficient rejection rate for urea, rendering it unsuitable for dialysis water recovery. Although there are elaborate enzymatic techniques capable of clearing dialysate such that it can be reused on patients, the filters and cartridge required for them are very expensive. Regions of significant indigence in combination with water scarceness cannot afford such techniques.
Dialysis with patient’s intrinsic water
Dr. Goldau is therefore investigating another variant called cryo-purification, which is based on freeze concentration known from beverage industries. The aim is to reclaim more than 90% of the water extracted from patients using this method. The idea is to upconcentrate toxins to only those two or three liters of water per day that are to be eliminated anyway during every dialysis. Patients can refill this water by drinking. The remainder – generally 25 to 30 liters per day – is cleared and fed back to dialysis. “In our experiments the volume of water that has to be discarded is less than 10 percent. This amount is required to filter the toxins. Thus, when it comes to upconcentration our technique is almost as effective as the kidneys themselves,” says Goldau. In this way, the researcher and his team want to establish an adequate dialysis that uses the patient’s own water resources without dehydration. Expensive filters and cartridges would no longer be required.
But how does the cryo-purification work? It takes advantage of the ice crystals capability to exclude all previously dissolved contaminations. They are repelled to the surface of the crystal. “The ice crystals formed when water freezes have the ability to simultaneously expel impurities. This permits to separate all the uremic toxins – i.e. metabolic waste products that the body needs to eliminate via the urine,” explains Goldau. This procedure can be implemented within washcolumns that are customary at beverage or chemical industries. For mobile dialysis, a small wash column is sufficient to produce 30 to 40 ml/min of dialysate. To prepare fresh dialysate, only a small amount of energy is required. The electricity could arbitrarily be drawn from mains, a car battery or solar panels. A respective lab demonstrator with a chiller is being constructed and a patent application has been filed for the process. The researchers are currently working on an automated solution, for the development of which they still need support from industrial partners.
Wearable kidney for home dialysis
“Our form of dialysis can even be designed to be mobile – wearable hemodialysis would be feasible.” In the vision of the Rostock-based researcher the patient is provided with a vascular access via which the blood and the excess water are extracted and returned. This is connected to a vest with a dialysis filter membrane, which contains disposable water chambers of up to 4 liters of volume. Every two or three hours the patient connects the vest to a non-stationary base unit, which flushes the waste dialysate and refills fresh water, both within the same period it takes a healthy individual to visit the toilet.
Current dialysis in hospitals puts a huge strain on the body and greatly affects the quality of the patients life. According to studies, only between 20 and 40 percent of patients are still alive after ten years. With long-term dialysis that is tap-water independent and can be performed anytime at home or at work, the morbidity rate and the costs of dialysis could be reduced. In addition it would be available to people within the drought belts worldwide as well. Another advantage is that dialysis centers and hospitals could reduce their water costs. Goldau estimates that his process could save 90 percent of the water – and thus also the waste water – used for dialysis, as it is in a reclamation cycle. “Most of the water is recycled.” The physicist expects that the system can be market-ready within around five to seven years from the start of development.